Joint Replacement Rehab Protocol
What is a Total Knee Replacement (TKR)?
A total knee replacement (TKR) is a surgical procedure used to treat patients with moderate-to-severe, “bone on bone” osteoarthritis of knee. This is the joint surface between the “shin bone” (tibia) and the end of the “thigh bone” (femur) and between the “kneecap” (patella) and the femur. A TKR is a complete resurfacing/ replacement of the damaged surfaces of the knee joint with metal components and a polyethylene spacer.
WHO IS A CANDIDATE FOR A TOTAL KNEE REPLACEMENT (TKR)?
Patients who are candidates for a TKR are those with moderate-to-severe osteoarthritis of the knee and who have failed conservative/non-operative treatments. Conservative treatments include weight loss, physical therapy, braces, ambulatory aids, anti-inflammatory oral medications, and injection treatments (cortisone, hyaluronic acid, etc.) Patients with moderate-to-severe arthritis often present with symptoms of knee pain with activity with accompanying, swelling, stiffness, and decreased mobility that may improve with rest or lessened activity. Patients may also experience a crunching or grinding sensation when the knee moves.
Total knee replacements are most commonly performed in patients ages 50 and older. This procedure is, however, performed in younger patients based on medical necessity. To determine whether or not you are a candidate for a TKR, your surgeon will first obtain plain x-rays to assess areas of bone-on-bone arthritis. Your surgeon may then have you get an MRI to evaluate all other parts of your knee.
WHAT IS A CUSTOM TOTAL KNEE REPLACEMENT? IS IT NECESSARY?
Although knee replacement surgery is highly successful and durable, patient dissatisfaction has been reported to be anywhere from 20-25%. Complaints include the sensation that the knee feels “fake”, moves unnaturally, feels tight and stiff with residual pain.
This is not too surprising when you consider that the knee is an asymmetric joint and the standard “off-the-shelf” (OTS) replacements are symmetric and only available in certain sizes. The surgeon must shape the bones to the closest size fit of the implant available and loosen the soft tissues that are tight to “balance” the soft tissues around the knee. If the OTS implant is a close fit and the soft tissues are properly balanced, the patient will do well. This is similar to how an “off-the-rack” suits fits average size people but fails to fit very small or large people. Whereas a “bespoke” custom-tailored suit will always fit well no matter the size of the person. Custom-made implants use 21st century technology now only available because of enhanced software development and ‘printing’ technology.
A custom-made knee replacement is individualized to only one patient. A CT scan is taken of the entire affected leg to allow software engineers to print’ individualized jigs for the surgery that will restore the leg alignment to be straight and not ‘knock kneed’ or ‘bow legged’.
The software engineers then use the images of the knee to restore the exact shape of the knee before it became arthritic and print individualized molds of the knee. These molds are made precisely to fit that individual patient and no one else.
As the knee has 2 weight bearing surfaces at different levels from each other, 2 plastic inserts are made to restore the exact joint line level as the patient originally had. These plastic inserts use vitamin E infusion patented technology that has a 40% improved wear rate over standard plastic inserts. Restoring the original form leads to better movement, function, and satisfaction. Other benefits to custom total knee replacements are:
- Thinner implants with 40% less bone removed
- Less bleeding
- Excellent return of motion earlier
- Patient satisfaction has improved from 80+% to mid-90%
Software engineers’ depiction of an exact fit, asymmetric, individualized, custom-made knee replacement
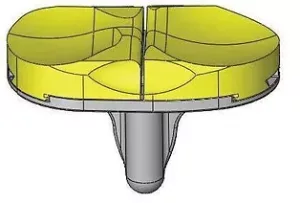

Custom-made knee replacement made from exact fit printed molds, restoring the patient’s knee joint surfaces precisely to what they originally were. (Made from cobalt chrome metal and vitamin E infused polyethylene)

Femoral Component (Cobalt chromium)
Articulating Surface (Polyethylene)
Stemmed Tibial Plate (Cobalt chromium)
Stem (Cobalt chromium)
